Epilepsy and the gut in dogs: microbiome and epileptic seizures
If your dog suffers from epilepsy, you have probably already heard about antiepileptic medications, neurological check-ups, and the occasional anxious moment in the vet’s waiting room. What you may not have been told yet is that your dog’s gut could be playing a role in all of this. This is not speculation: it is the subject of a growing line of research, with a peer-reviewed study published in 2025 in Research in Veterinary Science (The fecal metabolome and microbiome are altered in dogs with idiopathic epilepsy compared to healthy dogs) that adds concrete data to what was already suspected.
What is the microbiome and why does it affect canine epilepsy
The gut microbiome is the community of billions of bacteria, viruses and fungi that live in your dog’s digestive tract.
It is not an inert mass: it interacts with the immune system, metabolism and, in an increasingly well-documented way, with the brain.
Dogs with epilepsy frequently show dysbiosis — an imbalance in the composition of this microbial community compared to that of healthy dogs.
The interesting point is not just that the difference exists, but that it may not be a simple consequence of the disease: it could actually be contributing to it.
Bacteria, neurotransmitters and the seizure threshold
Gut bacteria produce and influence neurotransmitters such as GABA and serotonin. GABA in particular is the brain’s primary inhibitory neurotransmitter: when it functions properly, it dampens neural excitability.
When the microbiome is disrupted, this regulation can lose efficiency. Added to this is inflammation. A dysbiotic gut tends to release pro-inflammatory molecules into the bloodstream that reach the central nervous system.
Chronic inflammation lowers the seizure threshold: the brain becomes more reactive, easier to “ignite”.
Beneficial bacteria also produce short-chain fatty acids (butyrate, propionate, acetate) that have documented neuroprotective effects.
They protect the blood-brain barrier, stabilise nerve transmission and reduce neuroinflammation.
When those bacteria decline, so does this protection.
The 2025 study: probiotics may reduce seizure frequency
The study published in Research in Veterinary Science in 2025 analysed the effect of probiotic supplementation in dogs with epilepsy.
The result: dogs receiving probiotics showed a statistically lower seizure frequency compared to the control group.
This is not the first study to suggest this link, but it is one of the most recent and methodologically robust.
The researchers also observed that multi-strain Lactobacillus blends tend to produce better results than single strains.
The hypothesised reason is that they act on multiple points of the gut-brain axis simultaneously — a synergistic effect that a single bacterium alone cannot replicate.
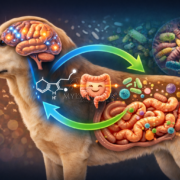
What is meant by the gut-brain axis?
The gut-brain axis is not a metaphor: it is a real network of nervous, hormonal and immune connections linking the gastrointestinal tract to the central nervous system.
The vagus nerve is the main pathway, but not the only one. Signals travel in both directions: the brain influences the gut (anyone who has experienced digestive issues during stress knows this well) and the gut influences the brain.
In epileptic dogs, this bidirectional channel can become a problem: a dysbiotic gut sends the wrong signals to an already vulnerable nervous system.
Ketogenic diet and microbiome: an approach still under study
Ketogenic diets — high in fat and protein, low in carbohydrates — have been used for decades in human paediatric epilepsy with documented results.
In dogs, research is still preliminary, but available data suggest that these diets modify the microbiome in a way that is favourable to seizure control.
The mechanism could be twofold: on one hand, the ketone bodies produced by lipid metabolism have a direct effect on neuronal stabilisation; on the other, the diet selects a different gut bacterial composition, with possible benefits for inflammation and neurotransmitter production.
A word of caution, however: a ketogenic diet for a dog cannot be improvised — it requires precise veterinary formulation and careful monitoring, especially in animals already on drug therapy.
What does all this mean in practice
Gut-targeted therapies do not replace antiepileptic medications.
No study has yet demonstrated that probiotics alone can adequately control canine epilepsy.
What does emerge, however, is that the gut microbiome may be an additional point of intervention, integratable into the overall management of the disease.
In practice this means:
- Discussing with your vet the use of multi-strain Lactobacillus-based probiotics as a supplement to standard therapy
- Paying close attention to diet quality, avoiding foods that promote dysbiosis (excess sugar, low fibre, poor-quality ingredients)
- Never independently changing your dog’s diet or discontinuing medication without consulting a veterinary neurologist
Frequently asked questions about epilepsy and the microbiome in dogs
What is gut dysbiosis in an epileptic dog?
Dysbiosis is an imbalance in the composition of the gut microbiome. In dogs with epilepsy, a reduction in beneficial bacteria such as Lactobacillus is frequently observed, along with an altered balance between different microbial populations, with documented effects on the gut-brain axis.
Can probiotics reduce epileptic seizures in dogs?
A 2025 study published in Research in Veterinary Science found an association between probiotic supplementation and lower seizure frequency in epileptic dogs.
The best results were observed with multi-strain Lactobacillus blends.
Does the ketogenic diet work for dogs with epilepsy?
Preliminary data are promising, but not yet conclusive.
It may be considered as additional support under strict veterinary supervision.
It cannot be improvised and does not replace drug therapy.
How do gut bacteria influence a dog’s brain?
They produce and stimulate the synthesis of GABA and serotonin, regulate systemic inflammation, and generate short-chain fatty acids with neuroprotective effects. When the microbiome is disrupted, these mechanisms function less effectively.
Should I speak to my vet before giving probiotics to my epileptic dog?
Yes. Probiotics are not inherently dangerous, but in a dog taking antiepileptic drugs the management must be coordinated.
Your vet can recommend the most suitable formulation and incorporate this approach into the existing treatment plan.
Is your dog suffering from epileptic seizures?
Every dog is different, and canine epilepsy requires a personalised approach.
If you are looking for information on how to support your dog with an integrated approach combining natural nutrition and a healthy microbiome, contact us at 391 18 92 137 for specialist nutritional advice and to move away from any source of processed commercial food.